Nigeria carries the world’s highest burden of obstetric fistula. Two recent reports from Nigeria Health Watch and Doctors Without Borders/Médecins Sans Frontières describe a growing network of surgical care, financial protection, and community outreach that is beginning to make a difference.

In northern Nigeria, a woman can labor for days without skilled help nearby. If the baby becomes lodged in the birth canal long enough, the sustained pressure causes tissue to die, opening a hole between the vaginal wall and the bladder or rectum.
The result is obstetric fistula — continuous leakage, chronic discomfort, and, for most women who develop it, a slow withdrawal from ordinary life. They stop going to markets, to worship, to family gatherings. Many are divorced. Some describe the years before repair as a kind of living disappearance.
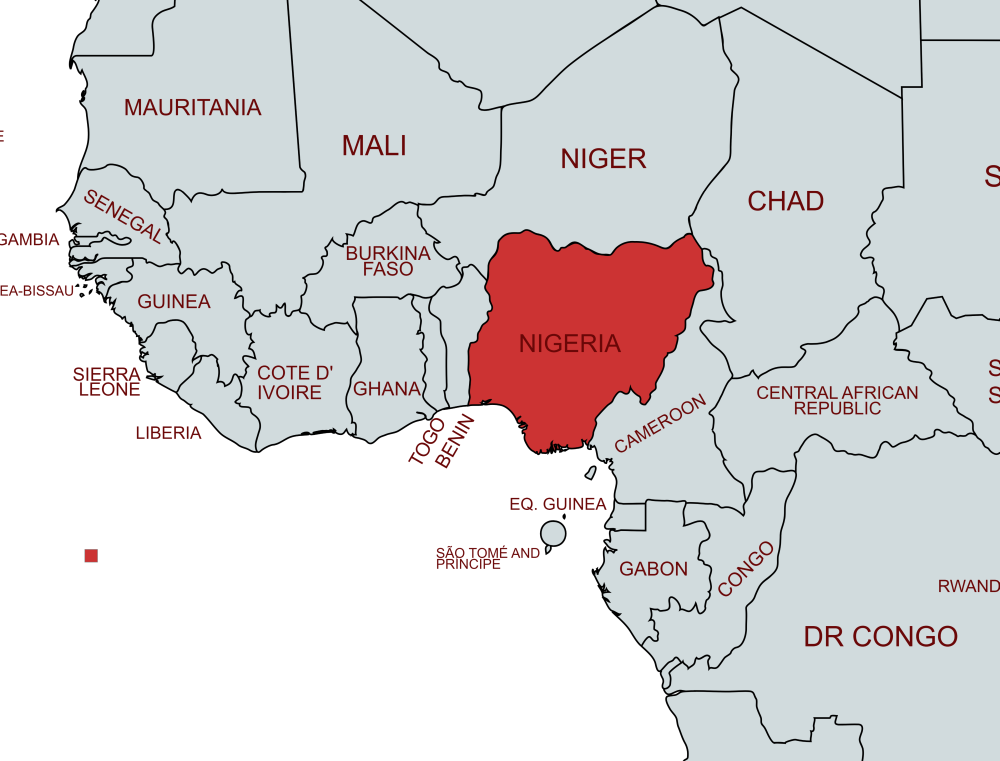
Nigeria carries the heaviest global burden of obstetric fistula, a fact that is less surprising when set against the country’s broader health landscape. Only 43% of births are attended by a skilled professional. Female literacy rates sit below 50%. Regional conflict, rural poverty, and an overwhelmed health system compound the problem at every level.
Two recent reports, from Nigeria Health Watch and Doctors Without Borders/Médecins Sans Frontières (MSF)— document what serious, sustained intervention looks like, and where the limits of that intervention still lie.
Expanding Coverage
Since June 2024, Nigeria’s National Health Insurance Authority has operated a fistula programme across 18 facilities that covers surgery, transportation, feeding, and post-operative care at no cost to patients.
But the programme’s more distinctive feature is what it does after surgery. Beneficiaries are enrolled in Nigeria’s broader health insurance framework, with coverage extended to their spouses and children under 18. In a country where more than 70% of health expenditure comes out of pocket, according to World Bank data, that extension of coverage represents something more than a medical benefit: it pulls women and their families into a system they have largely been excluded from.
In Ebonyi State, approximately 79 women have been enrolled in the health insurance scheme following fistula treatment. In Kano, 2,157 have benefited from the intervention.
Clinicians at both sites are emphatic that surgical repair is only the beginning. Women are counseled on family planning before discharge, and those who become pregnant again are directed to deliver by planned Caesarean section, since a vaginal delivery after repair can undo the surgery entirely.
The programme confronts real constraints. Fistula surgeons are scarce. At the Laure Fistula Centre in Kano, Dr. Amiru Imam Yola — who has performed more than 10,000 VVF repairs over 29 years — noted that trained specialists often leave when incentives are insufficient. Demand consistently outpaces capacity, and some women arrive after failed surgeries elsewhere, requiring more complex care.
Expanding the Network
At Jahun General Hospital in Jigawa State, MSF has operated a fistula ward since 2008, treating roughly 300 women a year in a 55-bed unit that functions, by design, as more than a surgical facility. Since 2024, the programme has added physical rehabilitation, training local physiotherapists to help women regain bodily control. This step is essential to restoring dignity, not just function, MSF has stated. Mental health support is integrated throughout.
MSF frames the larger challenge plainly: fistula is rare where cesarean sections are available. Ending it requires not just surgical capacity but political will, community engagement, and the kind of sustained investment in women’s health infrastructure that has so far been the exception rather than the rule.
The Fistula Foundation, working in Nigeria since 2010, launched a treatment network in 2025 with the goal of more than doubling annual surgeries — from 1,400 to 2,500 — by 2027, while training over 100 healthcare workers and deploying 200 community “fistula ambassadors” to identify and refer women in need.
Taken together, what’s emerging in Nigeria is something rarer than a single successful programme: a layered response, with surgical care, financial protection, rehabilitation, and community outreach reinforcing each other. More resources are certainly needed, but these reports demonstrate how much progress has already been made.
This summary is based on the following sources:
- Closing the Gap: Linking Fistula Surgery to Health Coverage in Nigeria, by Mahdi Garba and Tzar Oluigbo for Nigeria Health Watch
- A haven of recovery and support for fistula patients in Nigeria, from Doctors Without Borders/Médecins Sans Frontières
- Country Report: Nigeria, from the Fistula Foundation
Related Articles
Fistula Care Provides Healing for Women in Baidoa, Somalia
MSF opened a specialized fistula repair unit in Baidoa, Somalia, providing surgery and comprehensive care for women suffering obstetric fistula. The service addresses a critical gap, offering hope and dignity to women previously forced to travel to Mogadishu.

“Power of Joy”: New Film on Childbirth During Ethiopia’s Civil War
The documentary follows a girl who survived a harrowing childbirth to become an ambassador for women’s health. From Think Global Health.

Kristof’s Holiday Impact: Life-Changing Charities Transforming Healthcare in World’s Poorest Regions
The Fistula Foundation and Muso Health are revolutionizing healthcare delivery in developing nations, with the former providing critical surgeries for childbirth injuries and the latter deploying community health workers to reduce child mortality dramatically.

