MSF emergency services are helping women in hard-to-reach places access care.
First published September 27, 2023, by Doctors Without Borders/Médecins Sans Frontières
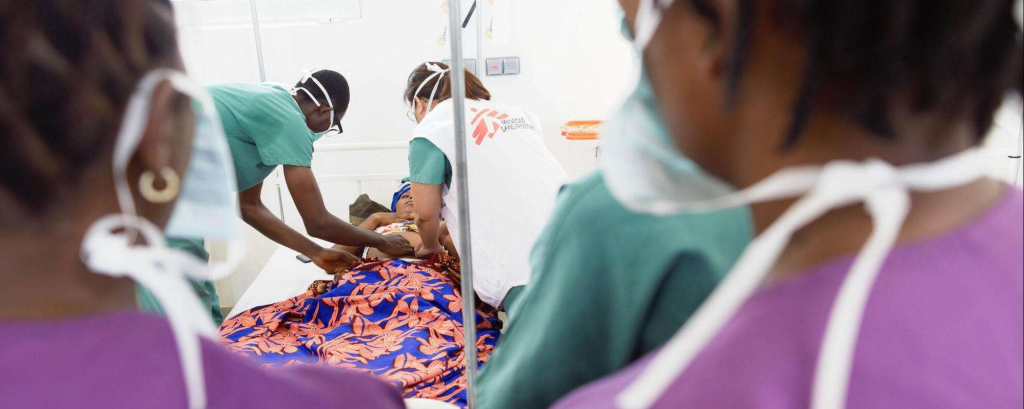
“When I went into labor, I started making my way to the nearest health center, but then I felt one of my two babies coming. So I spread a cloth under a mango tree and gave birth on my own.”
Musa Yahyah is a patient of Doctors Without Borders/Médecins Sans Frontières (MSF) in Sierra Leone, a country with one of the highest maternal mortality rates in the world. According to the World Health Organization, there are an estimated 443 deaths per 100,000 live births in the country. Many women there live in remote, rural areas that are located far from maternal health facilities, and they cannot afford the high cost of transport to reach a hospital.


“A traditional birth attendant helped me deliver the second baby under the mango tree,” Yahya explained. “Afterwards, she called a motorcycle-taxi to take me and my twins to MSF’s mother and child hospital in Hangha, because I was bleeding a lot. They gave me a transfusion of two pints of blood, then me and my babies were finally fine.”

MSF’s ambulance service steps in
MSF runs an ambulance service to get women and children in need of emergency care to hospitals as fast as possible.
“There is a significant need for ambulances to transfer pregnant women experiencing complications from local clinics to hospitals,” said MSF medical coordinator Kennedy Uadiale. “A good referral system is key and needs to be prioritized to save more lives.”
Between January and July 2023, MSF’s eight ambulances transferred 372 pregnant women and new mothers with their babies to a hospital for emergency care. The women faced a range of life-threatening conditions including pregnancy-induced hypertension, anemia, and hemorrhage. MSF also reimburses women for the cost of taking a motorcycle-taxi, the only alternative transportation available in most places, to health facilities. We funded 900 trips in the first seven months of 2023.
“I started experiencing labor pains at night,” said Umo Ngamanga, an 18-year-old from Moyamba district in Sierra Leone, “but to get to the health center in Foindu, which is 10 km [six miles] away, you have to walk for two hours as well as cross a river.” Ngamanga gave birth at home because she was unable to reach the nearest health center in time.
“My baby was not eating, and he had a fever, so the next day I took him to Foindu. He was immediately taken by motorcycle-taxi to Hinistas community health center, and then by MSF ambulance to Magburaka hospital. After receiving care, he got better, and I was able to bring him home.”

“Late referrals can be fatal”
Pregnant women in Sierra Leone must also contend with poor roads, a countrywide shortage of ambulances, and a lack of proper patient referral mechanisms. If a woman experiences complications during childbirth, it may be too late by the time she reaches a hospital.
“Late referrals can be fatal,” said Amadu Musa, an MSF nurse at Hangha hospital. “Some medical complications can be avoided if women with obstetric emergencies are able to reach health facilities on time. We had a patient from Daama village, about two hours from our hospital, who was pregnant and was referred very late. When the doctors did a scan, they found out that the baby did not have a heartbeat. The mother was also very anemic and in critical condition.”
“We had a patient from Daama village, about two hours from our hospital, who was pregnant and was referred very late. When the doctors did a scan, they found out that the baby did not have a heartbeat.”
–Amadu Musa, MSF nurse at Hangha Hospital
MSF’s team in Kenema carry out emergency Cesareans and other lifesaving surgeries for pregnant women and new mothers. MSF also has teams working in two other locations in Sierra Leone—Mile 91 and Magburaka, the latter in Tonkolili district—to help local health care providers respond to maternal and pediatric medical emergencies. In the first seven months of 2023, our teams in Sierra Leone helped 3,326 women deliver their babies, including 505 by emergency Cesarean.

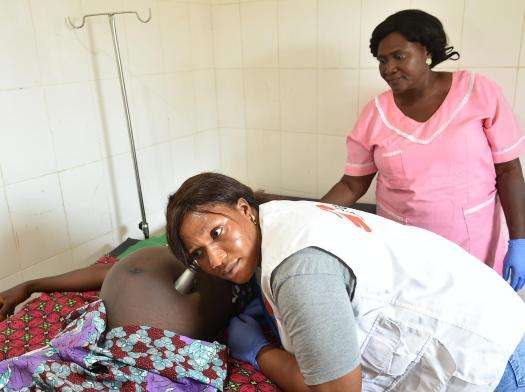
Expanded services are needed
MSF has also trained traditional birth attendants in Kenema district to monitor pregnant women and watch out for danger signs, referring them to the closest health center for medical attention, or calling an MSF ambulance to take them to a hospital if they need advanced care.
MSF teams in Sierra Leone are providing crucial care, but much more is needed if the country is to continue the progress made in the past 23 years.
“Health programming in the country needs to include staffing, maintenance, and fuel for ambulances at the National Emergency Medical Services,” said MSF head of mission Mohamed Morchid. “It is also important to consider creative and sustainable models supporting emergency transport needs from patients’ houses to their nearest health facilities, as this remains one of the main barriers identified by our patients in terms of their access to quality medical care. We encourage the Ministry of Health and Sanitation, as well as health and development partners and stakeholders, to make additional investments in emergency transport. This would help save many more lives.”
MSF in Sierra Leone
MSF has been working in Sierra Leone since 1986. In Mile 91 and Magburaka town, in Tonkolili district, MSF teams work with the Ministry of Health and Sanitation to provide medical care for mothers and children in local health centers and Magburaka hospital. In Hangha, Kenema district, MSF built a mother and child hospital, where teams provide comprehensive emergency obstetric and newborn care. In Makeni regional hospital in Bombali district, MSF teams provide treatment for patients with drug-resistant tuberculosis.
